Bill & Melinda Gates: Vaccine fairness will make us all safer | Free to read

Roula Khalaf, Editor of the FT, selects her favourite stories in this weekly newsletter.
The writers head the Bill & Melinda Gates Foundation
In this uncertain time, we know two things for sure: we want to end the Covid-19 pandemic as soon as possible, and we want to save as many lives as we can. That is why scientists everywhere are racing to create vaccines. Some countries are already buying up doses, even before the research and development is finished. But research released today shows that we must shift to a more co-ordinated approach soon, or we are all headed for a longer, deadlier pandemic.
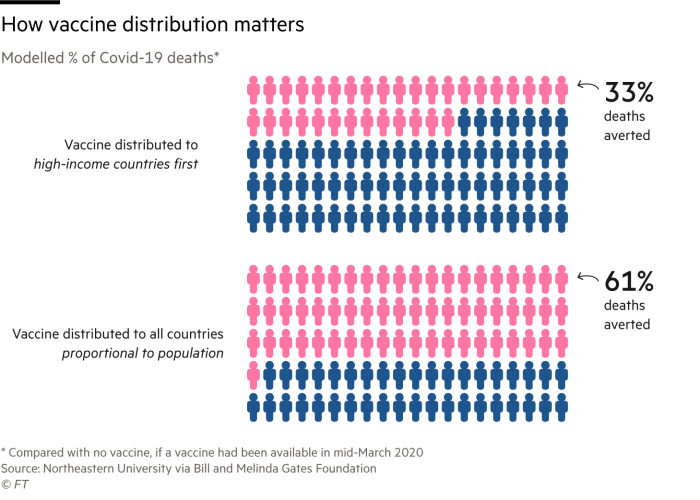
Our foundation asked modellers at Northeastern University’s Mobs Lab to consider two different scenarios. In one, approximately 50 high-income countries monopolise the first 2bn doses of vaccine. In the other, doses are distributed globally based on each country’s population, not its wealth.
The Mobs Lab team has modelled global influenza transmission for years, so they are well positioned to make Covid-19 predictions. The challenge this time is to account for the countless unknowns about the future course of this disease. There are no historical patterns to extrapolate from, so the team ran what are known as counterfactual scenarios, examining what would have happened if a vaccine had been available starting in mid-March.
Without an actual vaccine, they had to make some assumptions: specifically that a single dose of vaccine would be 80 per cent effective two weeks after administration, and 125m doses could be administered per week. But for the most part, their conclusions are based on observed data about what has already happened.
In the fairer scenario, a vaccine would have averted 61 per cent of the deaths through to September 1. In the less equitable scenario where rich nations hoard the vaccine, almost twice as many people die, and the disease continues to spread unchecked for four months in three quarters of the world.
Unfortunately, based on many wealthy countries’ behaviour so far, the hoarding scenario currently seems more likely. We understand the impulse to cut deals with pharmaceutical companies to reserve vaccine. Governments have a responsibility to protect the health of their people, and their investments can jump-start R&D and pay for manufacturing facilities. But we should not mistake a few bilateral transactions for an effective strategy.
The pandemic and the economic recession are global, and national solutions are inadequate. Borders are meaningless to pathogens and becoming less consequential to economies with each passing year. Consider New Zealand. It contained the disease well enough to get back to normal, jam-packed rugby stadiums included. But the economy still shrank, and the virus came back, and the country has had to shut down again.
The two of us are advocates for health equality. Our foundation fights diseases that kill millions because they are not top of mind in rich countries. When it comes to Covid-19, the poorest face the opposite problem: because it is centre stage in rich countries, the poorest may be sent to the back of the line.
However, this time there is no distinction between the moral argument and the self-interested one. Fair global distribution of Covid-19 vaccines would end the pandemic faster for everyone. And for every month we shave off, the world saves roughly $500bn, according to the IMF. If some nations are fully vaccinated, their economies will do a little better, but there is no scenario in which a few countries return to prosperity while the pandemic festers everywhere else, global supply chains stay broken and international travel is halted.
So what does an effective, equitable response actually look like?
Our foundation supports an initiative that brings together proven global health institutions to research and develop, manufacture, and deliver diagnostic tests, treatments, and vaccines. All countries that contribute to the vaccine portion, known as Covax, will be guaranteed access to successful vaccines in its portfolio in proportion to their at-risk population.
It has been encouraging to see the European Commission, South Korea, Japan, and several Middle Eastern countries express support for Covax. Momentum towards a multilateral solution is finally starting to build. But we will need more high-income countries to join in.
Latest coronavirus news
Follow FT's live coverage and analysis of the global pandemic and the rapidly evolving economic crisis here.
Countries that choose not to join Covax need to support a global response in other ways. They could set aside some of their reserved doses of vaccine for lower-income countries, as some did during the H1N1 pandemic. Or they can donate to Gavi, the vaccine alliance, which has two decades of experience helping lower-income countries deliver vaccines. Pharmaceutical companies must also make their products affordable for everyone during this crisis.
We believe global collaboration is the most effective way forward. Businesses and governments must understand that the future is not a zero-sum contest in which winners win only when someone else loses. It is a co-operative endeavour in which we all make progress together.
Letter in response to this article:
A different take on who should get the vaccine first / From Vic Paine, Derwen, Denbighshire, UK

Comments