Healthcare professionals demonstrate immunity to AI

Roula Khalaf, Editor of the FT, selects her favourite stories in this weekly newsletter.
When Robert Wachter, chair of the Department of Medicine at the University of California, San Francisco, reflects on the extent to which healthcare jobs will be disrupted by artificial intelligence, he recalls an apocalyptic speech given by the British-Canadian computer scientist Geoffrey Hinton.
Hinton sent shockwaves through specialist medical education with his warning in 2016: “We should stop training radiologists now. It’s just completely obvious that, within five years, deep learning is going to do better.”
The technology seemed so good that it would soon replace humans. But the reality has been rather different. Beyond a few applications — for example, in mammography and colonoscopy — evidence of AI’s superiority over doctors remains thin. Human intervention is still essential.
“Eight years out, we can’t hire enough radiologists, there’s so much demand,” points out Wachter, who is also a director of the Josiah Macy Foundation, which focuses on medical education. “AI is not perfect; and, in malpractice, you want to sue a human.”
AI has the potential to significantly transform employment in many aspects of healthcare — from basic research to clinical care, patient monitoring and medical administration. But Wachter’s comments are a reminder that its impact in transforming human roles and the timescales for such changes to take effect remain far from certain.
“I’m most impressed by our ignorance on AI,” says Wachter. “It has speeded up mammography, but there are lots of areas where it is not quite as good. Diagnosis is not just looking at digital dots but understanding and placing them in the clinical context. The number of scans is growing faster than AI is advancing.”
Use cases: drug development, compound identification, coding, data analysis
AI — and notably generative AI — offers considerable potential for improving treatments. Some breakthroughs have already been felt. In drug development, there has been much buzz around the identification of compounds such as treatments for antibiotic resistance. In 2021, a first practical example emerged of AI identifying a drug that has been put into practice: baricitinib, an existing treatment for rheumatoid arthritis was shown to be a way to treat complications of Covid-19.
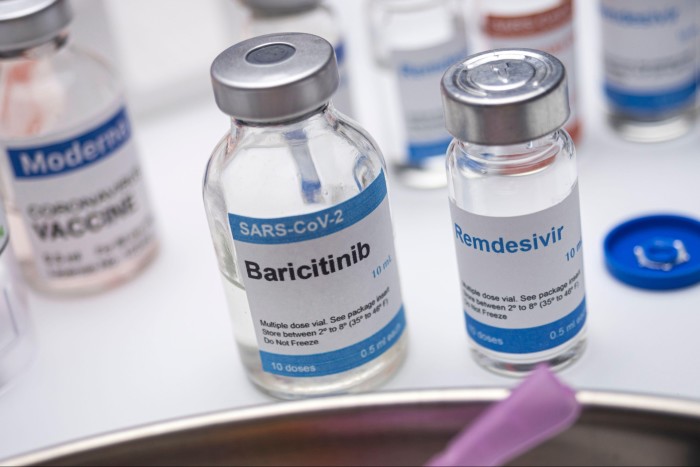
Overall, consultants McKinsey estimated in a report in January that AI could generate $60bn-$110bn a year for the pharmaceutical and medical-product industries by identifying compounds for possible new drugs, speeding their development and approval, and improving the way they are marketed.
McKinsey showed that since ChatGPT’s release in late 2022, the number of AI-related job listings has quadrupled. The number of positions offered grew by 43 per cent annually across the top 10 pharmaceutical companies alone since 2018.
The consultancy highlighted AI’s capabilities, including knowledge extraction, content and compound generation, customer engagement, and coding and software generation. McKinsey attributes these strengths to “gen AI’s truly multimodal nature: foundational models are built not just on language but also on images, omics [data analysis of an entire biological system], patient information, and other types of data”.
A report by the Brookings Institution pointed to AI’s roles in functions including post-treatment monitoring and follow-up, and in routine information gathering, particularly through the collection of information via chatbots by “engaging with patients in understandable language, resolving uncertainties, and summarising data for healthcare providers”.
Jobs enhanced: face-to-face consultations
Eric Topol, executive vice-president at Scripps Research, says: “AI is hugely transformational but these things always take longer than you might project.” Yet he already sees some applications elsewhere in his own medical practice.

These include note-taking in consultations — freeing doctors from their keyboards to spend more time and eye contact with patients. “That gives the physician the ability to get rid of all notes, tackle [their own] memory issues that are often a problem.”
Future doctors and other healthcare workers should not despair about their own displacement or redundancy. As a recent Pew Research survey highlighted, 60 per cent of Americans would be uncomfortable with their doctors or other providers relying on AI for their healthcare.
“We’ll always have human oversight — you are always going to want to talk to an experienced, empathetic physician,” says Topol. “Doctors, since before Hippocrates, ruled the roost and tended to be control freaks. The digital era has propelled the patient into a power position . . . we’re going to see that trend of democratisation get into high gear.”
He also sees technology driving changes to human medical recruitment, and training. “We were picking brainiacs to be physicians. We need people with deep empathy.” But he adds that far greater education is needed around AI. “It requires a reboot of our curriculum. There is no medical school in this country that has fully incorporated AI.”
Wachter adds: “I do believe that AI will be transformative, but healthcare is so stressed, [cash-]strapped and expensive that for the next 10 or 15 years it is unlikely whole medical groups will get fired. So much is wasteful, there is so much friction. Healthcare and education are the two fields that have been slowest for AI. There are no unemployed doctors or nurses.”

Comments