FT Health: Drug resistance, pandemics and the vaccination gap
Roula Khalaf, Editor of the FT, selects her favourite stories in this weekly newsletter.
Register here to receive your free weekly briefing by email.
There has been a near-epidemic spread in recent years of international meetings, conferences, grants, publications and declarations about the need to reduce use of antibiotics to avoid the development of drug resistance. Yet the latest stock-take makes for sobering reading.
A progress report published this week by the Food and Agriculture Organisation, the World Organisation for Animal Health and the World Health Organisation shows that fewer than 100 countries have a national action plan in place.
Most of these focus on human health, with only 64 nations limiting the use of antimicrobials in agriculture — an important factor driving resistance. More than a third reported no policy for the quality, sale and distribution of medicines. Yet the volume of antibiotics — and of reported resistance — continues to rise, while drug companies continue to reduce research for new treatments.
The analysis relies on “self assessment” by countries, which may not show the full picture. A new article in the Journal of Infection highlights that in many countries around the world, antibiotics are widely available through community pharmacies without prescriptions, even while on paper most nations require a doctor to prescribe them.
As the report on antimicrobial resistance concludes: “The real challenge now is to ensure that national action plans are not only developed but also implemented, funded and supported by monitoring and evaluation systems.”
Three questions
Stefan Elbe is professor of International Relations at the University of Sussex and author of the new book Pandemics, Pills, and Politics.
What is the principal conclusion of your book?
Developing new medicines and vaccines for use in global health emergencies — like pandemic flu and Ebola — is much more difficult than normal pharmaceutical development. This is important to recognise because many governments wish to secure their populations and economies against the shock of such deadly outbreaks by stockpiling medical countermeasures. The book identifies the ‘Top 10’ challenges involved, and shows what is being done globally to overcome them.
Was Tamiflu overhyped or did health authorities respond correctly at the time?
The Tamiflu ‘controversies’ [excessive stockpiling by the UK government] initially prompted me to write the book, but researching it persuaded me that health authorities had to perform a difficult task of balancing the publicly available scientific evidence with many things that cannot be known with certainty, as well as factoring in wider political considerations. There is so much more to the story than those public controversies, and we can learn much from the story about responding to future health emergencies.
What lessons should policymakers take for future pandemics?
First, normal processes of pharmaceutical development are unlikely to work for most new medical countermeasures so new economic and regulatory models are needed. Second, stockpiles only have limited use without parallel strategies for rapid distribution. Future outbreaks will continue to rely on a mix of pharmaceutical and non-pharmaceutical measures. Third, data transparency is absolutely critical for maintaining public trust during an emergency.
FT events
FT Pharma Pricing and Value Summit New York September 13. Details and tickets here — Discount of 20% for FT Health subscribers using code FTHEALTH.

Chartwatch
Vaccination gap Nine in ten of the world’s infants received at least one dose of vaccination against diphtheria-tetanus-pertussis in 2017, but 20m children still lack the full course needed to achieve universal coverage. 45m need a second dose of measles vaccine and 76m more need to be vaccinated with three doses of pneumococcal conjugate vaccine. (WHO, FT graphic)

News round-up
Aids warning The UN warned against complacency as the total number of people living with HIV rose to a record 36.9m with 1.8m people newly infected in 2017. Spending from donor governments rose last year mainly due to the timing of US contributions, but is set to decline. Another report said total global spending on HIV/Aids between 2000 and 2015 was $563bn. The head of the US flagship donor programme wants 70 per cent of funding to come from indigenous sources by 2030.
A new agreement with HIV drug suppliers aims to secure life-saving medicines for over 4m people. (FT, Kaiser Health, Lancet, Devex, Global Fund)
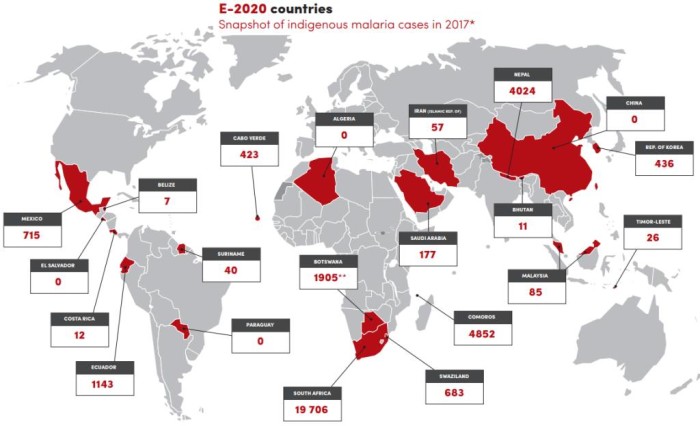
Measuring malaria A snapshot of the WHO campaign to defeat malaria in 21 countries by 2020 includes successful elimination in Paraguay. A new video game — Resistance 101 — is helping the fight. (WHO, Guardian audio)
The US and global health "If the people lose faith in government, science, and each other, the entire public health house of cards can quickly collapse," said one prominent commentator on the effect of Trumpian populism. The president's predecessor took a different tack, calling for more international co-operation to deal with situations such as pandemics. (Foreign Policy, Devex)
Security against smallpox The first drug to treat smallpox was approved by the US Food and Drug Administration. The move was seen as a protection against bioterrorism: the disease was wiped out in the 1970s. (NYT)
Chilling prospects As populations grow and the planet warms, billions of people are not able to cool down, hampering their ability to work, eat nutritiously and lead healthy lives. At immediate risk are 470m people in poor rural areas without access to safe food and medicines and 630m in hotter, poor urban slums with little protection against extreme heatwaves. (Sustainable Energy for All)

Mapping measles EU data on measles showed outbreaks continuing, notably in Romania, France, Greece and Italy, where political parties voicing anti-vaccination rhetoric have formed the country's new government. Only four European countries have reached the 95% vaccination target to stop transmission and festival-goers this summer have been warned to get jabs. A measles emergency has been declared in Brazil. (ECDC, Outbreak News)

Embryo ethics The Nuffield Council on Bioethics said editing the DNA of human embryos should be allowed, re-opening the debate about "designer babies". Any interventions "must be intended to secure, and be consistent with, the welfare of the future person, and they should not increase disadvantage, discrimination or division in society”. Here's the background to the debate. (FT, The Conversation)
Perishing polio A new book charts the rise and fall of the disease that caused widespread death and paralysis during the last century. Final attempts at eradication are proving difficult. Sudan has launched a campaign to vaccinate 3m children. (FT, VOA, Xinhua News)
Charting drug prices A new Bloomberg index measures price increases for some of the world's most widely-used drugs. Merck this week followed Pfizer and Novartis in halting price hikes on certain medicines. (Bloomberg, Stat)

Food insecurity New projections suggest food insecurity in poorer countries will fall from 21 per cent to 10 per cent over the next ten years, and the number of food-insecure people will drop from 782m to 446m. The measure is calculated by estimating the share of the population failing to reach a target of 2,100 calories per person per day — the level required to support an active lifestyle. (USDA, Devex)
Radiation row The mobile phone industry has been accused of casting doubt on scientific studies that suggest a link between cell phone use and cancer. A new study suggests radiation from phones may affect memory in adolescents. (Observer, Eureka)
Juul hits the UK Juul, the company that dominates the US ecigarette market, launched in the UK, targeting the country's 2.8m vapers. Back in the US it has faced criticism over its marketing and lobbying tactics. (FT, Wired)

Asthma alert New data showed asthma deaths in England and Wales has risen by 25 per cent over a decade as fears about air pollution intensify. Here's our podcast discussing the effects of air pollution on health. (The Guardian, FT)
Data danger A new analysis details the amount of personal information collected by US health insurers and how it affects what Americans pay for their coverage. Critics say using unverified "lifestyle" data to make medical assumptions means some could suffer unfair price rises or be unfairly discriminated against. (NPR/ProPublica)
Best from the journals
Dementia warning Nearly 50m people are living with dementia, and by 2030 this is expected to reach 82m, with the cost of support projected at $2tn. One year on from a WHO pledge to tackle the disease, little progress has been made. (The Lancet)
Media messaging Trials in Burkina Faso suggest mass radio campaigns in poorer countries can have significant effect in fighting diseases such as malaria, pneumonia and diarrhoea. (BMJ Global Health)
Cancer choices A new study highlighted the danger of those who ditched traditional cancer treatments for complementary therapies: they could be reducing their chance of survival. (Jama)
Tech troubles. The UK's new health secretary stressed the importance of tech in his first public speech on Friday, but criticism of services such as Babylon's virtual GP has led some to think the NHS is being too hasty.in adopting new services. (Ijndependent, BMJ)
Fishy business A new study says the omega 3 supplements taken by millions of people do not protect against heart disease. Omega 3 and fish-oil have long been touted as cardio-protective, with the result that Americans now get more omega 3 fats from supplements than they do from their diet. (Cochrane Library)
Podcast of the week
Overcoming AMR Doctors and vets discuss what they can learn from each other on tackling antimicrobial resistance. (BMJ Talk Medicine, 1 hour)
Join the debate
FT Health is free to read — please forward and encourage others to register here
Contact us via Twitter, Facebook, LinkedIn or email health@ft.com
Previous edition: Is there a doctor on board?
Latest news at www.ft.com/health and Twitter @FTHealth
Final thought
Corporate responsibility Morrisons, the UK supermarket chain, is introducing a "quiet hour" each week to help shoppers suffering from autism. Lights will be dimmed, music and tannoys silenced and checkout bleeps muted. What other measures should retailers take to cater for the varied needs of their customers?
Comments