Japan points the way in care for the elderly

Roula Khalaf, Editor of the FT, selects her favourite stories in this weekly newsletter.
Four years ago, health officials in Komagane in central Japan were wrestling with a persistent problem.
As in the rest of the country, the ski-resort city has a large elderly population — nearly a third of its 32,000 residents — for whom strokes are a significant health risk. Yet, in Komagane, the stroke mortality rate, particularly among women, was far above the national average.
The officials knew that stroke patients are at risk from a recurrence, with potentially deadly or debilitating consequences, and that lifestyle changes can cut that risk. But how to make that happen?
To address the problem, they embarked on a joint project with Komagane’s main hospital to provide preventive care and self-management support.
That scheme succeeded so well that Japan is now promoting it as a model for integrated healthcare across Asia. It also offers pointers for countries such as the UK, where the coronavirus pandemic has highlighted a need for deeper collaboration between different parts of the health and care system.
Japan, which has the highest proportion of elderly people in the world, has spent much of the past two decades trying to connect hospital treatment with broader prevention efforts and nursing care services.
In 2000, it introduced the Long-Term Care Insurance System, which is designed to finance long-term care for people over 65 — some 29 per cent of the population. Unlike the welfare schemes it replaced, it seeks to prioritise user choice and to integrate social and medical care. The number of people receiving benefits such as home visits and nursing care services has more than tripled since its introduction, to 6.7m.
Building on this system, the country began, from 2006, to adopt the so-called Community-based Integrated Care System. Under this initiative, municipalities will aim to co-ordinate public and private health services for old people by 2025, when the first cohorts of Japan’s baby boomers will have turned 75 or older. The aim is to enable the elderly to continue living in their communities while receiving long-term care.
“Japan has been hit by the double whammy of a rapidly ageing population as well as a declining birth rate,” an official at Japan’s health ministry says. “Our integrated care is a medium- to long-term effort to contain the risks, such as labour shortage, by having a community-based support system rather than depending on professionals alone.”
When city officials in Komagane first began working with Showa Inan General Hospital, the biggest hospital in the community, to put this policy into effect, it became clear that recurrences of strokes were a significant contributor to the city’s high stroke mortality rate. These, they found, were most likely to happen during the first year after a patient was discharged from hospital.
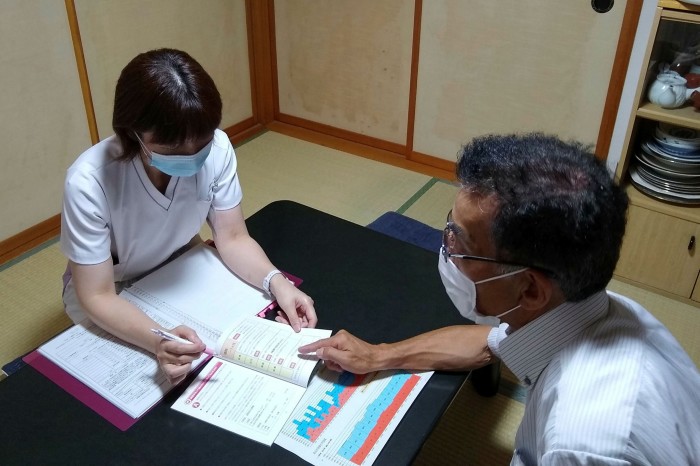
Under the joint programme devised by officials and doctors, stroke patients now compile plans to manage their health with support from nurses and nutritionists. After discharge, they are given pedometers to keep track of how much they are walking, and are asked to record their dietary habits and daily blood pressure in a notebook. Using this data, hospital staff follow up with patients for 12 months after discharge to ensure that they are sticking to their plans.
To make co-ordination easier, Komagane officials set up an office inside the hospital, allowing them to connect directly with elderly people requiring long-term care.
Their efforts have paid off. Hospital data show that the recurrence rate of strokes among patients within a year of discharge fell from 10 per cent in 2017 to 3 per cent in 2020.
Tatsuya Hama, a Komagane city official involved in the project, says the collaboration between the city and the hospital has brought benefits in other areas of healthcare. When the pandemic hit, for example, the city was able to co-ordinate with hospital staff to support Covid-19 patients and their families after discharge. “It became easier for us to identify the people who required support,” Hama says.
Other municipalities have seen similar benefits. “It’s not a coincidence that those who have long worked hard to provide home-based medical care to the elderly were able to support people who were recovering from Covid at home,” says Reisuke Iwana, senior analyst at think-tank Mitsubishi UFJ Research & Consulting. “The common issue is how communities can support the elderly.”
He warns, however, that the integrated care approach can also become a hodgepodge of local players from the private sector, non-profit organisations and hospitals — but without a central figure to co-ordinate the different layers of services.
Others point out that there are big disparities between communities that have been able to provide integrated services and others that have lacked the human and financial resources to do so.
Takako Tsutsui, an expert on care management for the elderly at the University of Hyogo, says such gaps were exposed during the pandemic as hospitals were forced to co-ordinate with nursing homes to take care of elderly Covid-19 patients.
“The collaboration between hospitals and nursing care homes deepened for those communities where managed care was functioning,” Tsutsui says. “But not for those who had no prior history of working together.”
Comments